MED INF 405 Health Care Information Tech Integration & Standards
|
Course Description
|
This course provides the details of health care technology standards and interoperability. Topics include the value proposition of standards; health information models; the IHE Initiative; HL7, DICOM, CCOW, CorbaMED, and other medical standards. The course also covers the role of nonmedical standards in medical informatics (HTTP, XML, etc.) as well as multi-institutional issues and telemedicine, e-commerce, and Health Insurance Portability and Accountability Act standards compliance.
|
|
Instructor: Julie Ann Bryant
|
|
Learning Goals
|
The goals of this course are to:• Describe the relevance of information architecture in health care organizations.
• Describe the benefits and challenges of standards-based HIT interoperability. • Describe principles of controlled standard terminologies. • Explore U.S. national and international interoperability standards. • Describe principles of health information exchange. • Analyze an information systems project to determine the appropriate utilization and integration of HIT standards. |
|
Text
|
None
|
Course Reflection:
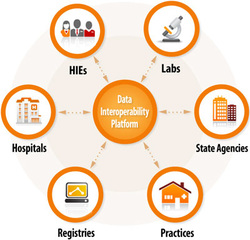
A complex health care system requires diverse electronic health record (EHR) products. One size does not fit all. To realize their full potential, EHR products must be able to share information seamlessly. An interoperable health IT environment makes this possible.
EHR Interoperability enables better workflows and reduced ambiguity, and allows data transfer among EHR systems and health care stakeholders. Ultimately, an interoperable environment improves the delivery of health care by making the right data available at the right time to the right people.
Where Standards Matter Most
In creating an interoperable health IT environment, standards are particularly critical in four areas of EHR technology:
The Nation's move toward a fully interoperable health IT environment is a work in progress, with new developments every day. It's important to keep in mind that older EHR systems may not be fully compatible with newer products. Systems that predate current standards may require installation of applications that function as translators.
In recent years increased focused has highlighted need for interoperability and standardization in health care information systems.
Interoperability — allows various software and hardware vendors to communicate across a multitude of platforms. The federal government, as led by the Health and Human Services Agency (HHS) is a leading proponent of electronic health records, for example, an executive order created the position of National Health Information Coordinator (http://www.healthit.gov/).
The desires for interoperable and standardized systems are apparent in all sectors of any health care organization. A surgeon operating on a patient would require immediate access to a patient’s history, medications, and recent lab test results in order to make the best determinations. During Postop the clinician needs to communicate the appropriate laboratory results to the patient’s primary care physician. It’s impractical for the surgeon to solely rely on the patient for all their medical history, collate their information from various disconnected information systems (IS), or wait for paper medical chart that in many circumstances could be missing some of this critical data. The system should spontaneously and impeccably share data across the healthcare organization and show it in advantageous ways.
Interoperability involves the construction, recognition, and application of clinical data standards to guarantee that information in one area of the enterprise is available and meaningful among a multiplicity of clinical settings. Standards are rules which dictate how patient data is electronically stored and communicated. Most standards are text, numerical, and image-based data and easily accessed and exchanged by health stakeholders – providers, payers, employers and patients.
Patient medical records are aggregation of exchanges among providers, patients, insurance companies, and government agencies. The information is usually unclassified text descriptions and images. Most times, clinical information standards are deemed as a complicated “alphabet soup” of various terminologies and ambiguous technical details
A complex health care system requires diverse electronic health record (EHR) products. One size does not fit all. To realize their full potential, EHR products must be able to share information seamlessly. An interoperable health IT environment makes this possible.
EHR Interoperability enables better workflows and reduced ambiguity, and allows data transfer among EHR systems and health care stakeholders. Ultimately, an interoperable environment improves the delivery of health care by making the right data available at the right time to the right people.
Where Standards Matter Most
In creating an interoperable health IT environment, standards are particularly critical in four areas of EHR technology:
- How applications interact with users (such as e-prescribing)
- How systems communicate with each other (such as messaging standards)
- How information is processed and managed (such as health information exchange)
- How consumer devices integrate with other systems and applications (such as tablet PCs)
The Nation's move toward a fully interoperable health IT environment is a work in progress, with new developments every day. It's important to keep in mind that older EHR systems may not be fully compatible with newer products. Systems that predate current standards may require installation of applications that function as translators.
In recent years increased focused has highlighted need for interoperability and standardization in health care information systems.
Interoperability — allows various software and hardware vendors to communicate across a multitude of platforms. The federal government, as led by the Health and Human Services Agency (HHS) is a leading proponent of electronic health records, for example, an executive order created the position of National Health Information Coordinator (http://www.healthit.gov/).
The desires for interoperable and standardized systems are apparent in all sectors of any health care organization. A surgeon operating on a patient would require immediate access to a patient’s history, medications, and recent lab test results in order to make the best determinations. During Postop the clinician needs to communicate the appropriate laboratory results to the patient’s primary care physician. It’s impractical for the surgeon to solely rely on the patient for all their medical history, collate their information from various disconnected information systems (IS), or wait for paper medical chart that in many circumstances could be missing some of this critical data. The system should spontaneously and impeccably share data across the healthcare organization and show it in advantageous ways.
Interoperability involves the construction, recognition, and application of clinical data standards to guarantee that information in one area of the enterprise is available and meaningful among a multiplicity of clinical settings. Standards are rules which dictate how patient data is electronically stored and communicated. Most standards are text, numerical, and image-based data and easily accessed and exchanged by health stakeholders – providers, payers, employers and patients.
Patient medical records are aggregation of exchanges among providers, patients, insurance companies, and government agencies. The information is usually unclassified text descriptions and images. Most times, clinical information standards are deemed as a complicated “alphabet soup” of various terminologies and ambiguous technical details